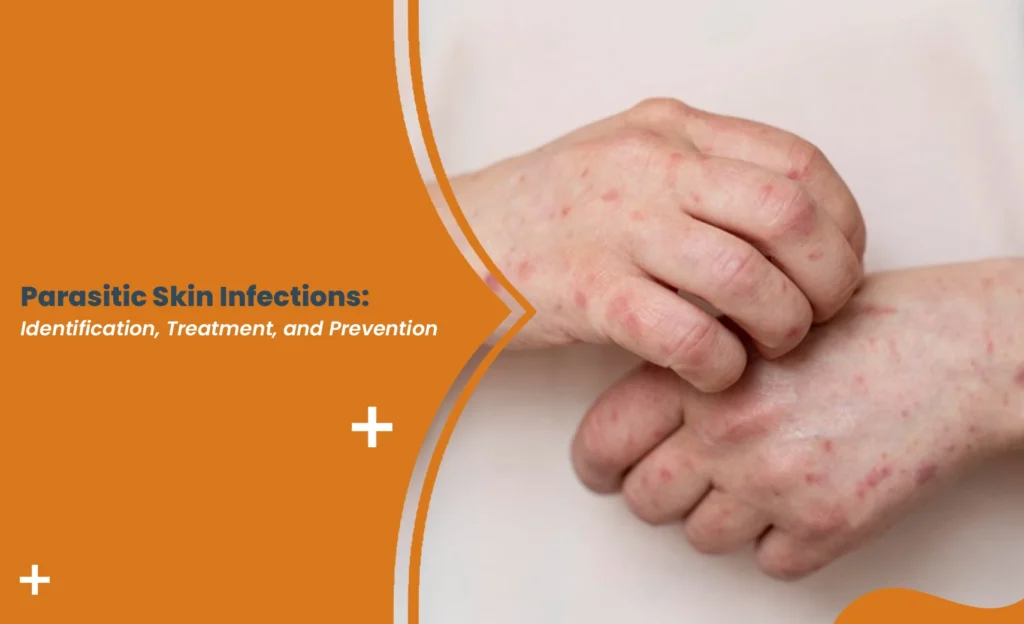
There’s something uniquely unsettling about a skin infection.
If it’s a sore throat, you can ignore it for a while. If it’s stomach pain, you can blame stress or last night’s takeaway. But when something appears on your skin – visible, itchy, persistent – it feels immediate. Personal. Almost invasive.
Parasitic skin infections carry that extra layer of discomfort. The idea that something microscopic is living on or beneath your skin isn’t just medically concerning. It’s psychologically disturbing.
And yet, they’re more common than we like to admit.
Not everywhere. Not constantly. But often enough that dermatologists in the US and UK see them regularly.
The good news? They’re identifiable. Treatable. Preventable.
The bad news? They’re easy to misdiagnose at first.
What counts as a parasitic skin infection?
When people think “parasite,” they usually imagine intestinal worms. But parasites don’t only target the gut.
Certain organisms prefer the skin.
Scabies, caused by microscopic mites burrowing into the outer layer of skin, is one of the most well-known examples. Cutaneous larva migrans – caused by hookworm larvae penetrating the skin – creates winding, itchy tracks that look almost like something drawn with a pen beneath the surface.
Then there are lice infestations, which technically fall under parasitic skin conditions too.
Each has its own pattern. Its own personality.
But they share one trait: persistent itching that doesn’t behave like normal irritation.
The early signs people miss
Parasitic skin infections rarely announce themselves dramatically.
It starts small.
An itch that doesn’t respond to moisturizer.
A rash that worsens at night.
Tiny bumps between fingers.
A creeping line under the skin after walking barefoot on a tropical beach.
Scabies, in particular, often causes itching that intensifies after dark. That detail alone has helped many clinicians narrow the diagnosis quickly.
I once interviewed a GP who said, “If someone tells me they’re itching worse at night and antihistamines aren’t helping, I immediately think of mites.”
And she was usually right.
Why they’re misdiagnosed
Many parasitic skin infections are initially mistaken for eczema, allergic reactions, or fungal rashes.
Topical steroids may temporarily calm inflammation – but they don’t eliminate the parasite.
The itching persists.
The rash spreads.
That’s often the turning point when patients seek further evaluation.
Diagnosis usually involves a physical exam. Sometimes a skin scraping under a microscope confirms the organism.
It’s not a dramatic process. Just precise.
Treatment options that actually work
Here’s where medicine steps in confidently.
Scabies, for example, is often treated with topical permethrin cream. But in certain cases – especially widespread or crusted scabies – oral medications may be prescribed.
That’s where treatments like Wormectin 12mg enter the conversation.
Wormectin 12mg contains ivermectin, which works by interfering with the nervous system of parasites like mites. It doesn’t soothe the skin directly. It targets the organism causing the problem.
For some patients, a single dose of Wormectin 12mg followed by a repeat dose after one to two weeks clears the infestation effectively.
But medication alone isn’t enough.
The importance of environmental control
With parasitic skin infections, treatment must extend beyond the body.
Clothing, bedding, towels – all require washing in hot water. Vacuuming furniture matters. Close contacts may need simultaneous treatment even if asymptomatic.
If Wormectin 12mg is prescribed for scabies, doctors usually emphasize environmental hygiene just as strongly.
Because reinfection isn’t uncommon when cleaning is skipped.
The organism is small.
But its ability to linger is impressive.
Cutaneous larva migrans: the beach souvenir nobody wants
This infection often appears after walking barefoot in sand contaminated by animal feces – usually in tropical or subtropical regions.
It creates snake-like red tracks under the skin. Intensely itchy.
It’s self-limiting in many cases – the larvae eventually die. But symptoms can last weeks without treatment.
Oral ivermectin-based therapy, such as Wormectin 12mg, may be prescribed to accelerate resolution. In many patients, itching improves within days after taking Wormectin 12mg.
Travel history often provides the clue here.
The rash isn’t random.
It tells a story.
Lice and social stigma
Lice are parasitic, yes. But they carry disproportionate embarrassment.
Head lice spread easily among children through close contact. They aren’t a sign of poor hygiene. They’re a sign of proximity.
While topical treatments remain first-line, resistant cases may require oral therapy. In some instances, physicians may consider ivermectin-based medications like Wormectin 12mg under appropriate supervision.
Again – context determines treatment.
Not panic.
Side effects and safety
For most healthy adults, Wormectin 12mg is generally well tolerated when prescribed correctly. Mild dizziness or nausea may occur. Severe reactions are rare under medical supervision.
Pregnancy requires caution. Children require weight-based dosing.
Precision protects safety.
Self-diagnosing and self-medicating complicate outcomes.
Testing first remains wise.
Prevention: boring but powerful
Preventing parasitic skin infections isn’t complicated.
Avoid walking barefoot in areas with uncertain sanitation.
Don’t share clothes or bedding with people who are sick.
Keep up with your regular cleaning in shared living areas.
If someone in your home has scabies, treat everyone in the house at the same time.
Small habits interrupt transmission.
And most importantly – early evaluation prevents spread.
If itching persists beyond a week without clear explanation, don’t just switch creams.
Ask questions.
A personal reflection
Years ago, I spoke with a college student who delayed treatment for scabies because she was embarrassed.
She thought it meant she was unclean.
By the time she sought help, half her dorm floor was itching.
The solution was straightforward: topical therapy, a dose of Wormectin 12mg, coordinated cleaning, and communication.
The hardest part wasn’t the parasite.
It was the silence.
When to see a doctor
Seek medical evaluation if:
- Itching is intense and persistent
- Rash worsens at night
- Skin shows burrows or tracks
- Travel history aligns with exposure
- Household members develop similar symptoms
If a parasitic skin infection is confirmed, your doctor may recommend Wormectin 12mg depending on severity and organism.
Treatment is usually simple.
Delaying it isn’t.
Final thoughts
Parasitic skin infections feel invasive because they are.
But they’re not a moral failure. Not a lifestyle indictment. Not a sign of neglect.
They’re biological events.
Identification requires observation.
Treatment requires precision.
Prevention requires small habits.
When appropriate, medications like Wormectin 12mg provide effective relief.
And relief often comes faster than people expect.
The fear fades.
The skin heals.
Life resumes.
Quietly.
FAQs
1. How do I know this isn’t just eczema or dry skin?
That’s the hardest part – early symptoms can look similar. The clue is persistence and pattern. If the itching is intense, spreads to close contacts, or gets noticeably worse at night, it’s worth getting checked. Eczema usually responds at least a little to moisturizers or mild steroid creams. Parasitic infections tend to ignore them. When in doubt, a quick doctor’s visit beats weeks of guessing.
2. I feel embarrassed even thinking about this. Should I?
Honestly? No. Parasites don’t choose based on cleanliness or social status. Scabies spreads through close contact. Lice spread in classrooms. Hookworm larvae live in sand, not in “dirty” people. The stigma is louder than the biology. Doctors treat these cases routinely – without judgment.
3. If I start treatment, how quickly will the itching stop?
This is where expectations matter. Even after the parasite is killed, itching can continue for a couple of weeks. That doesn’t necessarily mean treatment failed. Your immune system is still reacting to what was there. The rash fading gradually is normal. Instant relief is nice – but not always realistic.
4. Do I really need to wash everything in my house?
Not everything. But bedding, towels, and recently worn clothes should be washed in hot water if scabies or lice are confirmed. It’s less about deep-cleaning your entire life and more about interrupting the parasite’s ability to reinfect. Think targeted hygiene, not obsessive sterilization.
5. When should I worry that it is something more serious?
If the rash spreads quickly, hurts instead of itching, shows signs of infection (like fever or pus), or doesn’t go away after treatment, see a doctor. Most parasitic skin infections are straightforward. But symptoms that don’t go away or get worse need to be looked at again.

